Science has marched on: it’s time to update the advice to Canadians
 A year ago we reported on the scientific progress that had been made since 2018, when the National Academies of Science, Engineering and Medicine (NASEM) issued its conclusions on the Public Health Consequences of E-cigarettes.
A year ago we reported on the scientific progress that had been made since 2018, when the National Academies of Science, Engineering and Medicine (NASEM) issued its conclusions on the Public Health Consequences of E-cigarettes.
This post provides a further update on key research findings, offering further evidence for our governments to stop suggesting that “the long-term consequences of vaping are unknown” and instead acknowledge that we now know that commercial products cause specific and severe damage to users.
The NASEM conclusions were founded on less than one-third of the evidence now available.
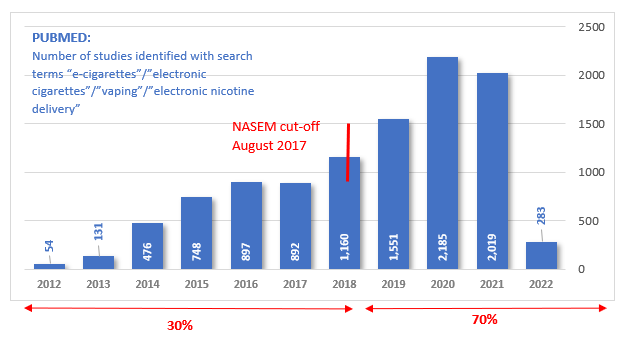
The NASEM report was commissioned by the U.S. Food and Drug Administration in 2016. The committee looked at literature that was indexed for publication before August 31, 2017. Of the more than 10,000 articles indexed on PUBMED mentioning e-cigarettes or vaping, more than two-thirds have been published AFTER the committee had released its conclusions.
The NASEM committee acknowledged that it did not have sufficient evidence to address many questions about conclusions were founded on less than one-third of the evidence now available.
The NASEM panel of experts explored the scientific evidence behind 47 conclusions, finding that there was conclusive or substantial scientific evidence for only 18, moderate evidence for 8, and limited to no evidence for 21. Fifteen of the 18 conclusions for which there was strong or substantial level of confidence confirmed potential harms from these products and only two related to potential benefits of vaping. These were the committee’s conclusions that e-cigarette users who abandoned tobacco were exposed to fewer of the chemicals found in cigarette smoke and that these former-smokers who vaped experienced short-term health consequences in some organ systems.
Since 2018, other governments have assigned committees of scientists to conduct reviews of the growing body of evidence. From these, a scientific consensus is emerging that vaping is dangerous and not especially useful as a smoking cessation method. While no single authoritative document has brought together these systematic reviews, meta-analyses and report of health authorities, it is not apparent that:
- E-cigarettes have increased the number of young nicotine users in some countries.
- Young people who use e-cigarettes are more likely to smoke conventional cigarettes.
- Dual use is common and harmful.
- When purchased as consumer products, e-cigarettes are not effective cessation aids.
- E-cigarettes cause damage to respiratory and circulatory systems.
- Other governments have provided more recent scientific assessments.
- Health Canada’s messaging on e-cigarettes is out-dated. .
 #1 E-cigarettes have increased the number of young nicotine users in some countries.
#1 E-cigarettes have increased the number of young nicotine users in some countries.
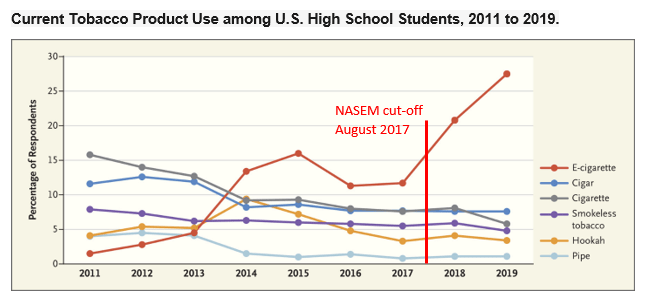
Their lack of attention to this health issue may be because at the time of their literature review, the ‘youth vaping epidemic’ had not yet been recognized. JUUL – the high-nicotine/high-fashion product that fueled the epidemic had its major launch in the summer of 2017 – only a few months before NASEM’s evidence cut-off.
After the NASEM report was published, it became evident that e-cigarettes had increased the number of American teenagers hooked on nicotine. By 2019, one-quarter of U.S. high school students were vapers. [A]
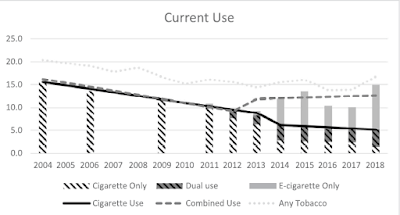 Vaping products reversed the downward trend in youth nicotine use. That is the key finding of a study by MeLisa Creamer and colleagues [B] that analyzed data from the US National Youth Tobacco Survey, conducted annually from 2004 to 2018 among a representative sample of US middle school and high school students. While cigarette use declined, e-cigarette use increased markedly. The net effect was more nicotine users in high schools. This was true both for ever use and current use of nicotine, as shown in the graphs below. By 2019, 15% of American high school students were current nicotine users.
Vaping products reversed the downward trend in youth nicotine use. That is the key finding of a study by MeLisa Creamer and colleagues [B] that analyzed data from the US National Youth Tobacco Survey, conducted annually from 2004 to 2018 among a representative sample of US middle school and high school students. While cigarette use declined, e-cigarette use increased markedly. The net effect was more nicotine users in high schools. This was true both for ever use and current use of nicotine, as shown in the graphs below. By 2019, 15% of American high school students were current nicotine users.
In Canada, the rate of nicotine use continues to be high. Data from the 2020-2021 Canadian Tobacco and Nicotine Survey (CTNS) [C ] confirm that one in seven teenagers and young adults (14% and 13% respectively) is a past-month vaper, and that one-third of high-school age kids have tried nicotine. These numbers underestimate the problem among 17-19 year-olds, as they include the younger ages (15 and 16) where prevalence is lower. Larger surveys of Canadian youth allow a closer look at each grade, and show that the child who enters high school in grade 9 as likely as not to have tried vaping before graduating. [D]
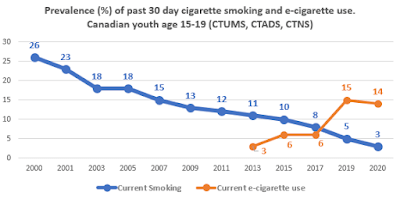 E-cigarettes are now the main product that is getting kids hooked on nicotine. The decline in cigarette smoking among young Canadians, for example, reflects a shift in the products they are recruited to use, not a decrease in initiation.
E-cigarettes are now the main product that is getting kids hooked on nicotine. The decline in cigarette smoking among young Canadians, for example, reflects a shift in the products they are recruited to use, not a decrease in initiation.
#3 Young people who use e-cigarettes are more likely to smoke conventional cigarettes
The NASEM committee found “moderate” evidence that young people who used e-cigarettes were more likely to subsequently smoke cigarettes.
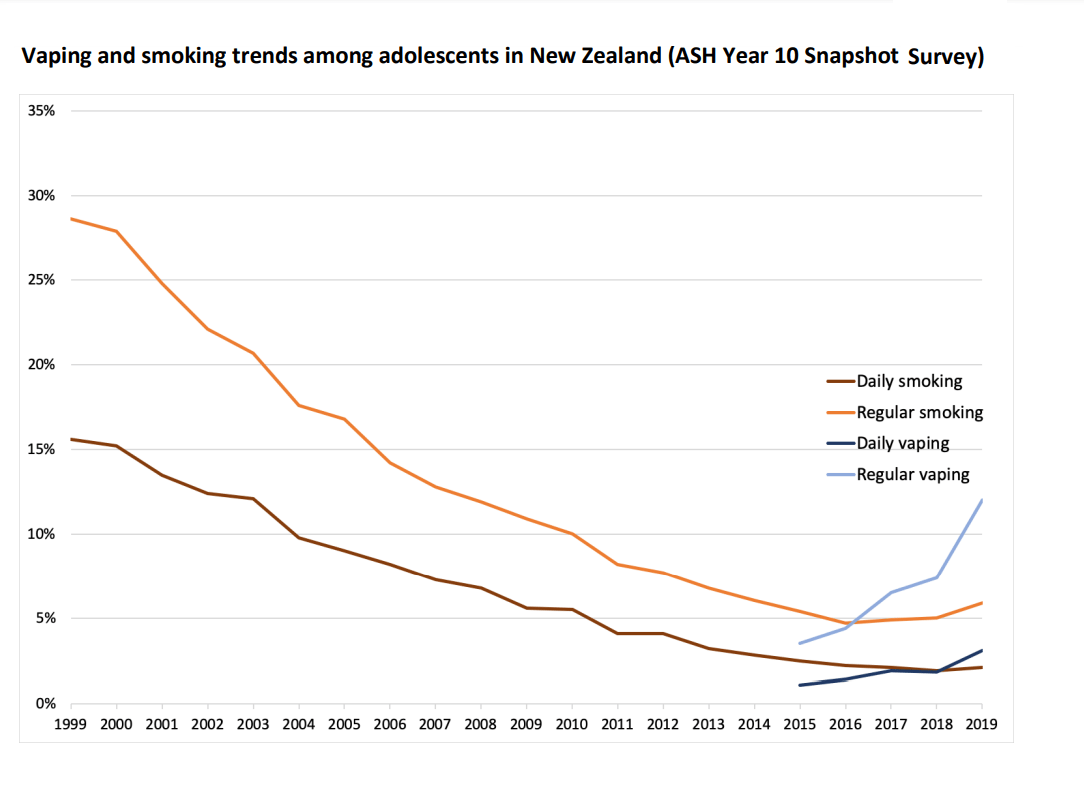 It is now better understood that young e-cigarette users are 3-4 times more likely to become cigarette smokers than adolescent non-users of nicotine. This increased susceptibility, combined with the large number of young vapers, raises concerns that we may see a reversal of the downward trend in youth vaping. This appears to have already happened in another country with relaxed vaping regulations. In the most recent cycle of the Year 10 school survey, as reported by New Zealand’s ASPIRE 2025 research team [E] both cigarette smoking and vaping had risen.
It is now better understood that young e-cigarette users are 3-4 times more likely to become cigarette smokers than adolescent non-users of nicotine. This increased susceptibility, combined with the large number of young vapers, raises concerns that we may see a reversal of the downward trend in youth vaping. This appears to have already happened in another country with relaxed vaping regulations. In the most recent cycle of the Year 10 school survey, as reported by New Zealand’s ASPIRE 2025 research team [E] both cigarette smoking and vaping had risen.
Multiple studies have now confirmed that adolescents who use e-cigarettes are at least three times more likely to take up smoking than non-users of e-cigarettes. Significant reviews and meta-analyses which confirm this association include a systematic review and meta-analysis conducted by researchers based in Australia, using studies that were published before October 2020. Sze Lin Yoong and colleagues restricted their analysis to longitudinal studies only, thus strengthening the certainty of the findings. Their meta-analysis of 17 such studies of e-cigarette use at baseline and subsequent ever cigarette use ( found a relative risk of cigarette uptake of 3.01. All 17 studies showed a positive relationship. [F]
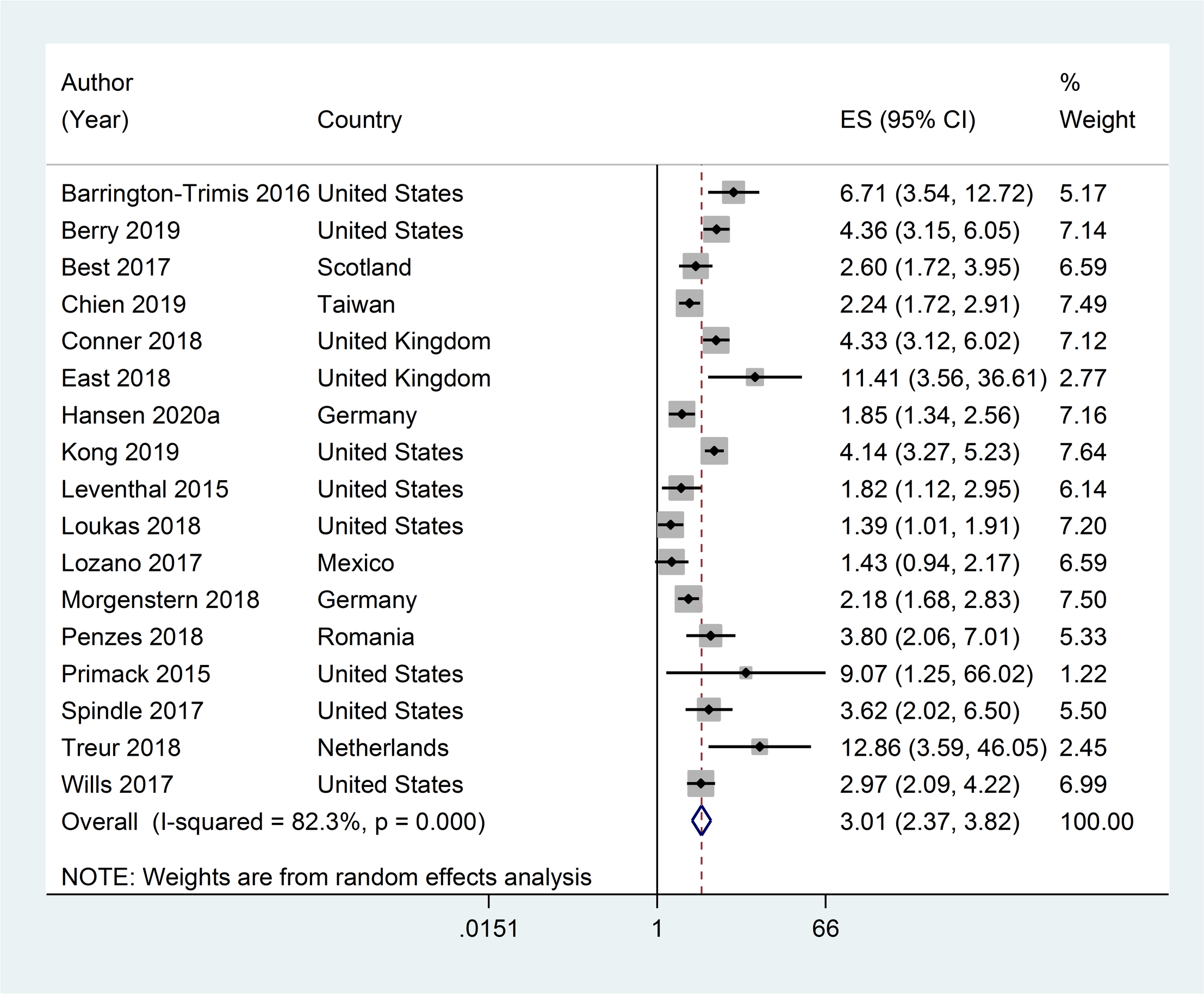 This study builds on the conclusions of other recent meta-analyses, including those published 2020 by British researchers (Kouja et al. based on evidence up to November 2018) [G] and another Australian team (Baenziger et al. based on evidence up to April 2020). [H]
This study builds on the conclusions of other recent meta-analyses, including those published 2020 by British researchers (Kouja et al. based on evidence up to November 2018) [G] and another Australian team (Baenziger et al. based on evidence up to April 2020). [H]
And newer studies provide consistent results. After the October 2020 cut-off date for the Yoong meta-analysis, more longitudinal studies appeared were published that provide consistent conclusions.
In July 2021, Jeremy Staff and colleagues reported on their study using longitudinal data on British youth who were questioned at age 14 and followed at age 17. They found that young people who were using e-cigarettes at age 14, but not smoking, were more than five times more likely to have started smoking tobacco cigarettes by age 17. The reverse was true too. Those who started smoking tobacco cigarettes at age 14 were three times more likely take up e-cigarettes by age 17. Their results counter the proposition that the young people who vape would otherwise be smokers (the ‘common liability’ theory) as they found distinct risk factors for tobacco-use and vaping. [I]
Also in July 2021, a paper written by the Netherlands’ research team lead by Thomas Martinelli reported on e-cigarette use and tobacco smoking among Dutch-speaking high school students in the Netherlands and Belgium. [J] This longitudinal study collected follow-up information after six and twelve months and found that those who were using e-cigarettes were 5.63 times more likely to be using tobacco a year later. They also found that those who were smoking tobacco were 3 times more likely to be using e-cigarette at the year’s end. These findings are very like those of British youth reported by Staff et al., cited above.
A few weeks earlier, Elizabeth Hair and colleagues reported on a longitudinal study of youth and young adults (15-21 year-olds in 2017) who were contacted after one year. This study found that users of e-cigarettes in 2017 were more than three times more likely to become users of cigars, little cigars or cigarillos (CLCCs) by 2018. Young people who were cigarette smokers or marijuana users in 2017 were also more likely to become users of CLCCs by 2018. [K]
California researchers lead by John Pierce analyzed data from 4 waves of the American longitudinal PATH study, finding that e-cigarette use tripled the risk of becoming a daily smoker over the period of the data collection. [L]
#3 Dual use of combustible cigarettes and e-cigarettes is common and harmful
Health Canada’s vaping web page provides the optimistic proposition: “There are short-term general health improvements if you completely switch from smoking cigarettes to vaping products.” [M]
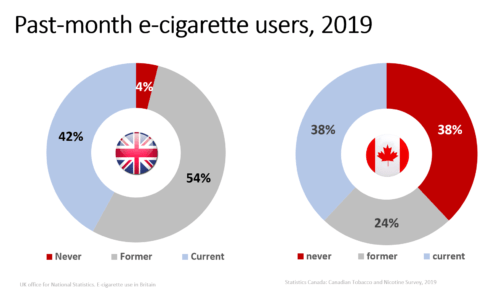 The problem with this proposition in Canada is that only one-third of vapers are smokers who “completely switch.” A much larger proportion (38%) are people who both smoke and vape. [C] (Data from the Canadian Tobacco and Nicotine Survey and the U.K. Office for National Statistics are shown below).
The problem with this proposition in Canada is that only one-third of vapers are smokers who “completely switch.” A much larger proportion (38%) are people who both smoke and vape. [C] (Data from the Canadian Tobacco and Nicotine Survey and the U.K. Office for National Statistics are shown below).
Researchers using data from heart studies [N, O] and general population studies have concluded that using both e-cigarettes and conventional cigarettes is likely more harmful than only smoking or only vaping. [P]
#4 When purchased as consumer products, e-cigarettes are not effective cessation aids.
The NASEM committee concluded that “There is moderate evidence from randomized controlled trials that e-cigarettes with nicotine are more effective than e-cigarettes without nicotine for smoking cessation.”
A number of studies have been published since then which emphasize the difference between real-world use of these products and the results in clinical settings. It is becoming clear that e-cigarettes used as consumer products are not effective as smoking cessation devices, while e-cigarettes given therapeutically in controlled clinical settings may help some people quit smoking.
As a recent Cochrane review explains it: “key questions about e-cigarettes mainly lie outside the realm in which randomized controlled trials (RCTs) are useful, and relate to the population impact of policies that promote their use for people who smoke compared with alternative policy positions that try to restrict their use…. increasing rates of continued use and use by people who have never smoked show that there is also potential for population harm.” [Q]
A number of research teams have identified very different results for e-cigarette use in real-world settings than in clinical contexts. Key studies include a meta-analysis published in January 2021 by Richard Wang and associates, [R] which collected data from studies published up to January 2020, including 55 observational studies and 9 randomized control trials (RCTs). The study found that overall e-cigarettes, as consumer products, are not associated with increased smoking cessation in the adult population, although in randomized control trials, provision of free e-cigarettes as a therapeutic intervention was associated with increased smoking cessation.
This analysis confirmed the trend found in analyses of longitudinal data from the United States, (some reported here earlier). In February 2022, Ruifeng Chen and colleagues used more recent waves of the PATH study and found that smokers trying to quit using e-cigarettes were 7% less likely to succeed than those using other methods of quitting.[S]
New research is showing that “normal” or “typical” use of e-cigarettes is not associated with success. A longitudinal survey in the United Kingdom found that daily e-cigarette users were significantly more likely to quit smoking than were people who were using NRT or going “cold turkey”, while non-daily e-cigarette users were significantly less likely to quit smoking than people using other methods or no method at all. More than half (60%) of all e-cigarette users were in the category of less-successful non-daily. [T] Other researchers have found similar associations. [U]
A 2021 meta-analysis by Zhang and colleagues [V] with data from 35 studies also found an association with intensiveness of e-cigarettes use or clinical settings and success. (A secondary finding was that adolescent e-cigarette users were three times more likely to become cigarette smokers, consistent with the data reported above). [E to L]
Additional concerns about ‘typical’ use of e-cigarettes by former smokers include the increased chance of relapse to smoking cigarettes. A small number of studies have been directed at this consequence (as reviewed by a Brazilian research team led by Laura Barufaldi).[W They found smoking relapse was twice as likely among people who had quit smoking but subsequently started using e-cigarettes.
#5. E-cigarettes cause damage to respiratory and circulatory systems.
The NASEM committee found very little published science on which they could assess whether e-cigarettes caused significant harm to the respiratory, heart or other body systems. The absence of knowledge at that time was the basis of the take-away from the report that the ‘long-term consequences of vaping were unknown’.
It is now known that there are significant long-term health risks associated with these products. Since the NASEM report, there have been hundreds of studies published that have examined adverse health consequences of e-cigarette use using laboratory studies of animals and humans. Studies on animals and human tissue have lead researchers to conclude that the damage caused by e-cigarettes is the type that leads to lung and heart disease and strokes.
A useful such summary was published in March 2021 by two American researchers who reviewed the Cardiovascular and immunologic effects of electronic cigarettes. [X] (References cited in the paper are hyper-linked)
In summary, the weight-of-evidence discussed above warrants the view that the use of e-cigarettes has multiple adverse health effects. Acute use of e-cigarettes leads to an increase in heart rate and blood pressure [40], as well as obstruction of conducting airways [39], and arterial stiffness [61]. Flow-mediated dilation is diminished [69], transcutaneous oxygen tension is decreased [106], and a characteristic immune response [40, 41, 81] is activated. Chronic use of e-cigarettes has been found to be associated with a shift in cardiac autonomic balance towards sympathetic predominance [64] and dysregulation of immune-related genes [82]. In animal models, long-term exposure to e-cigarette aerosols lead to DNA damage and inhibition of DNA repair and the development of adenocarcinoma and bladder urothelial hyperplasia [28]. Lipid-laden macrophages accumulate in the lung, accompanied by extensive changes in lipid metabolism and transport [100]. Taken together, these observations raise the possibility that habitual use of e-cigarettes could cause tissue injury, which could compromise lung function and increase the risk of developing heart disease and stroke. The use of e-cigarettes could also compromise the ability to remove microbial pathogens and thereby increase susceptibility to viral, fungal, and bacterial infection. Data from experimental models also support the notion that the use of e-cigarettes could increase the risk of developing several types of cancer. Nevertheless, it remains to be seen whether long-term use of e-cigarettes is indeed associated with such adverse events in humans.
Similar findings have been made by other research teams:
In January 2020, Buchanan et al., in their comprehensive review of cardiovascular effects reported “…recent studies have also suggested that e-cigarette use is associated with inflammation, oxidative stress, and haemodynamic imbalance leading to increased cardiovascular diseases risk.” [Y]
In 2019, Kennedy et al., in their review of 38 studies of cardiovascular effects of e-cigarettes reported, “Most studies suggest potential for cardiovascular harm from electronic cigarette use, through mechanisms that increase risk of thrombosis and atherosclerosis.” [Z]
In 2020, Wills et al. reported the results of a review and meta-analyses of respiratory effects of e-cigarettes. They showed that e-cigarette use was associated with a 39% increase in the risk of asthma and a 51% increase in the risk of chronic obstructive pulmonary disease. They also concluded; “Laboratory studies consistently show an effect of e-cigarettes on biological processes related to respiratory harm and susceptibility to illness.” [AA]
The work by Wills et al. extended the 2019 review by Gotts et al. of the respiratory effects of e-cigarettes. At that time, Jeffery Gotts and his colleagues concluded: “Studies show measurable adverse biologic effects on organ and cellular health in humans, in animals, and in vitro.” [AB]
More recent 2021 reviews and studies have confirmed and updated the findings of the works discussed above. Stella Tommasi and colleagues further investigated gene dysregulation in smokers and vapers. They found that genes that control mitochondria (Mitochondria are cells’ energy factories. Their disruption is an early sign of long-term disease development.) were disrupted both by smoking and vaping. While there was some overlap, there many cases of dysregulation that were vape-specific and others that were tobacco-specific. [AC]
Lauren Davis and colleagues published a review of the pulmonary effects of long-term e-cigarette use early in 2022 that updated earlier reviews of the respiratory effects of e-cigarettes. Davis and colleagues concluded: “Chronically, these changes are likely to result in irreversible parenchymal lung tissue damage and impaired gas exchange, contributing to chronic lung conditions in long-term vapers.” [AD]
While not a review article, the 2022 report by Poonam Rao and colleagues adds to our understanding of how e-cigarette vapour impairs vascular functioning. In a 2022 study, the researchers showed that a wide range of e-cigarettes impaired blood flow in mice (as measured by flow-mediated dilation) in much the same way and to approximately the same degree as combustible cigarettes. [AE]
#6 Other governments have provided more recent scientific assessments than NASEM.
The NASEM committee was one of the earlier scientific panels established by government health authorities to review the science related to e-cigarette regulation. Since then a number of other governments or inter-governmental organizations have commissioned reports. Except for reports from the United Kingdom (Public Health England, National Institute for Health and Care Excellence), that continue to recommend e-cigarettes for smoking cessation, at least eight other recent national and intergovernmental reports conclude that e-cigarettes are hazardous and are not recommended for smoking cessation.
The European Commission. A year after the NASEM report was published, the European Union asked its scientific advisers (the Scientific Committee on Health, Environmental and Emerging Risks – SCHEER) to provide an opinion three aspects of e-cigarettes: their use and adverse effects, and their role as a ‘gateway’ to smoking. With their cut off date of April 2019, this committee had 9 more months of evidence to consider than did the NASEM committee. After making their preliminary assessment available for public input and reviewing comments, SCHEER adopted its “Final Opinion on Electronic Cigarettes” last year (April 2021). [AF]
This report strengthens concerns about the risks associated with e-cigarette use, while failing to find more than weak evidence that they help smokers quit. SCHEER concluded:
- evidence supporting e-cigarettes as an effective smoking cessation device was “weak”.
- evidence that second-hand exposure to e-cigarette vapour posed risks was “weak to moderate”.
- evidence that e-cigarettes helped smokers cut down on the amount smoked was “weak to moderate”.
- evidence that e-cigarettes could cause cancer in the respiratory tract was “weak to moderate”.
- evidence that e-cigarettes posed risks for coronary disease was “moderate”.
- evidence that e-cigarettes were a gateway to smoking for young people was “moderate”
- evidence that e-cigarettes with nicotine were addictive was “strong”
- evidence that flavours in these products contribute to initiation was “strong”.
Other American scientific committees. In January 2020, the U.S. Surgeon General issued a report on smoking cessation, in which the efficacy of e-cigarettes to aid quitting attempts was reviewed based on evidence published into 2019. The report found that this assessment was made more difficult because of the wide variety of products that were in the market, and that “there is presently inadequate evidence to conclude that e-cigarettes, in general, increase smoking cessation.” [AG] The following year, in January 2021, the United States Preventive Services Task Force also recommended against counselling smokers to use e-cigarettes. “The USPSTF concludes that the current evidence is insufficient to assess the balance of benefits and harms of e-cigarettes for tobacco cessation in adults, including pregnant persons. The USPSTF recommends that clinicians direct patients who use tobacco to other tobacco cessation interventions with proven effectiveness and established safety.” [AH]
Review commissioned for the Irish government. In June 2020 the Irish Health Research Board reported on its assessment of scientific papers published until February 2020 that addressed the effectiveness of e-cigarettes as cessation products [AI] and the role they played in the initiation of conventional cigarette smoking by adolescents. [AJ] In these two reports. that “e-cigarettes were not more effective for smoking cessation than approved nicotine replacement therapies (NRTs), which questions the need for e-cigarettes as a smoking cessation intervention. In the second review, we found that e-cigarettes were associated with initiation of conventional cigarette smoking among adolescents, which identifies a potentially serious harm.”
Review commissioned for the Spanish government. Spain’s public health agency concluded in 2020 that “To date, no toxicological or drug studies have been performed on the long-term safety of e-cigarette use in humans; without these data it is impossible to say with certainty that e-cigarettes are safer than cigarettes. With this in mind it is impossible to recommend these devices as a useful tool against the cessation of traditional tobacco consumption.” (machine translation) [AK]
Review commissioned for the Australian government. The Australian National Centre for Epidemiology and Public Health concluded that e-cigarettes did not help people quit smoking, but did increase the probability of a young person starting to smoke.[AL] (The evidence review was separately published.) [H]
For the Netherlands government, the Trimbos Institute reviewed the literature and found that e-cigarettes were effective as cessation products for only a small group of smokers, and that success rates were comparable to “regular” methods. Because most e-cigarette users in that country also continued to smoke, it cautioned about the additional risks of dual use. [AM]
At the request of the French government, the French High Council for Public Health reconsidered its 2016 conclusion that e-cigarettes were a useful tool to help people quit smoking. After reviewing new evidence, they issued a revised finding in November 2021: “Evidence-based knowledge in insufficient to propose to health professionals that they use electronic nicotine delivery systems to help thier patients quit smoking.” [unofficial translation].[AN]
 #7 Health Canada’s messaging on e-cigarettes is outdated.
#7 Health Canada’s messaging on e-cigarettes is outdated.
Unlike the governments cited above, Health Canada has not updated its assessment of the risks of vaping for several years, and cites no research on risks or cessation more recent than 2018.
Despite the accumulating evidence to the contrary, the department continues to encourage smokers to believe that “using e-cigarettes is linked to improved rates of success,” [M] Despite the accumulating evidence of specific and serious long-term consequences, it continues to make its primary preventive message that “The long-term health impacts of vaping are unknown.” [AO]
While ALL the long-term effects of vaping are yet to be documented, it is no longer accurate to suggest that such effects are not known. The short-term adverse health effects are known and that these short-term impacts will almost certainly lead to long-term increases in the risk of disease and death among addicted vapers who continue to vape throughout their lives.
While some of the early adverse health effects identified in recent research are unique to vaping, broadly speaking, the same classes of adverse health effects occur when people start smoking combustible cigarettes. Our long experience with cigarette smoking has taught us that these early physiological changes inevitably lead to higher risks of disease and death from heart disease, stroke, lung diseases and cancer among those who continue to smoke. And, because of nicotine addiction, a great many people who started to smoke at a young age continue to smoke throughout their lives.
E-cigarettes contain nicotine and, like combustible cigarettes, are highly addictive. There is every reason to believe that the adverse health effects that have been observed in mostly young vapers will lead to higher risks of disease and death later in life among those who continue to vape. The tragic slow-acting epidemic of smoking-related disease and death after decades of smoking will almost certainly be repeated, perhaps only approximately, among those who continue to vape throughout their lives.
So the true meaning of sentence “The long-term health impacts of vaping are unknown” is that the short-term adverse health effects are known and that these short-term impacts will almost certainly lead to long-term increases in the risk of disease and death among addicted vapers who continue to vape throughout their lives.
Statements like this made by health authorities allow manufacturers to further minimize the risks of using their products, encourage smokers to use a cessation aid that for most will be less effective than traditional and safer products, and encourage young people and other users to think that vaping is a mostly harmless buzz-producing experience.
A more truthful, blunter message to young people is warranted. Something like: Smoking kills, and vaping almost certainly kills too.
And for smokers who are trying to quit on their own? Health Canada should advise: using e-cigarettes will likely decrease the chances of success but will increase health risks in comparison with approved smoking cessation aids.
Publications cited
[A] King BA et al. The EVALI and Youth Vaping Epidemics — Implications for Public Health. New England Journal of Medicine. February 20, 2020. https://www.nejm.org/doi/full/10.1056/NEJMp1916171#article_references
[B] Creamer ME et al. Effects of e-cigarette use on cigarette smoking among U.S. youth, 2004–2018. Preventive Medicine. Volume 142, January 2021, 106316. https://www.sciencedirect.com/science/article/abs/pii/S0091743520303406?via%3Dihub.
[C] Physicians for a Smoke-Free Canada. The Canadian Tobacco & Nicotine Survey, 2020-21. http://www.smoke-free.ca/SUAP/2021/CTNS-2020-results.pdf
[D] Health Canada. Summary of results for the Canadian Student Tobacco, Alcohol and Drugs Survey 2018-19. https://www.canada.ca/en/health-canada/services/canadian-student-tobacco-alcohol-drugs-survey/2018-2019-summary.html
[E] ASPIRE 2025. Submission on Smokefree Environments and Regulated Products (Vaping) Amendment Bill. https://aspire2025.files.wordpress.com/2020/04/aspire-vaping-bill-submission-final.pdf
[F] Yoong SL et al. Association between electronic nicotine delivery systems and electronic non-nicotine delivery systems with initiation of tobacco use in individuals aged < 20 years. A systematic review and meta-analysis. Plos One September 8, 2021. https://journals.plos.org/plosone/article/metrics?id=10.1371/journal.pone.0256044
[G] Khouja JN et al. Is e-cigarette use in non-smoking young adults associated with later smoking? A systematic review and meta-analysis. Tob Control. 2020 Mar 10;30(1):8–15. doi: 10.1136/tobaccocontrol-2019-055433. https://pubmed.ncbi.nlm.nih.gov/32156694/
[H] Baenziger ON et al. E-cigarette use and combustible tobacco cigarette smoking uptake among non-smokers, including relapse in former smokers: umbrella review, systematic review and meta-analysis, BMJ Open 2021. https://bmjopen.bmj.com/content/11/3/e045603
[I] Staff J et al. Adolescent electronic cigarette use and tobacco smoking in the Millennium Cohort Study. Addiction, 2021. https://onlinelibrary.wiley.com/doi/10.1111/add.15645
[J] Martinelli T et al. Exploring the gateway hypothesis of e-cigarettes and tobacco: a prospective replication study among adolescents in the Netherlands and Flanders. Tobacco Control Published Online First: 05 July 2021. https://tobaccocontrol.bmj.com/content/early/2021/08/18/tobaccocontrol-2021-056528
[K] Hair EC et al. A longitudinal analysis of e-cigarette use and cigar, little cigar or cigarillo initiation among youth and youth adults: 2017–2019. Drug and Alcohol Dependence, Volume 226, 2021. https://pubmed.ncbi.nlm.nih.gov/34218009/
[L] Pierce JP et al. Use of E-cigarettes and Other Tobacco Products and Progression to Daily Cigarette Smoking. Pediatrics January 2021, e2020025122; DOI: https://doi.org/10.1542/peds.2020-025122. https://publications.aap.org/pediatrics/article/147/2/e2020025122/36274/Use-of-E-cigarettes-and-Other-Tobacco-Products-and
[M] Health Canada. Vaping and quitting smoking. https://www.canada.ca/en/health-canada/services/smoking-tobacco/vaping/smokers.html
[N] Wang JB et al. Cigarette and e-cigarette dual use and risk of cardiopulmonary symptoms in the Health eHeart Study. PLOS One. July 25, 2018. https://doi.org/10.1371/journal.pone.0198681.
[O] Alzahrani T, Pena I, Temesgen N, Glantz S. Association between electronic cigarette use and myocardial infarction. American Journal of Preventive Medicine. 2018 October; 55(4): p. 455- 461.https://doi.org/10.1016/j.amepre.2018.05.004.
[P] Okunna N. A Comparison of Mental and Behavioral Health Risks Factors Associated With Current Dual Use of Electronic Cigarette and Conventional Tobacco Cigarettes With Exclusive Tobacco Cigarette Use and Nonuse Among Adults in the United States. American Journal on Addictions. 03 December 2020 https://doi.org/10.1111/ajad.1311
[Q] Livingstone-Banks J et al. Effects of interventions to combat tobacco addiction: Cochrane update of 2019 and 2020 reviews. Addiction 2021. https://onlinelibrary.wiley.com/doi/epdf/10.1111/add.15769
[R] Wang RJ et al. E-Cigarette Use and Adult Cigarette Smoking Cessation: A Meta-Analysis. American Journal of Public Health, https://doi.org/10.2105/AJPH.2020.305999
[S] Chen R et al. Effectiveness of e-cigarettes as aids for smoking cessation: evidence from the PATH Study cohort, 2017–2019Tobacco Control Published Online First: 07 February 2022. doi: 10.1136/tobaccocontrol-2021-056901
[T] McDermott MS et al. The effectiveness of using e‐cigarettes for quitting smoking compared to other cessation methods among adults in the United Kingdom. Addiction. 09 March 2021. https://doi.org/10.1111/add.15474
[U] Kasza KA et al. Association of e-Cigarette Use With Discontinuation of Cigarette Smoking Among Adult Smokers Who Were Initially Never Planning to Quit. JAMA Network. 2021.
[V] Zhang YY et al. The effect of e-cigarettes on smoking cessation and cigarette smoking initiation: An evidence-based rapid review and meta-analysis. Tob. Induc. Dis. 2021;19(January):4 https://doi.org/10.18332/tid/131624. http://www.tobaccoinduceddiseases.org/The-effect-of-e-cigarettes-on-smoking-cessation-and-cigarette-nsmoking-initiation,131624,0,2.html
[W] Barufaldi LA et al. Risk of smoking relapse with the use of electronic cigarettes: A systematic review with meta-analysis of longitudinal studies. Tob Prev Cessat. 2021;29:29. Published 2021 Apr 27. doi:10.18332/tpc/132964
[X] Keith R and Bhatnagar A. Cardiorespiratory and Immunologic Effects of Electronic Cigarettes. Curr Addict Rep. 2021 Mar 5:1-11. doi: 10.1007/s40429-021-00359-7. Epub ahead of print. PMID: 33717828; MCID: PMC7935224.
[Y] Buchanan N et al. Cardiovascular risk of electronic cigarettes: a review of preclinical and clinical studies, Cardiovascular Research, Volume 116, Issue 1, 1 January 2020, Pages 40–50, https://doi.org/10.1093/cvr/cvz256
[Z] Kennedy CD et al. The cardiovascular effects of electronic cigarettes: A systematic review of experimental studies. Prev Med. 2019 Oct;127:105770. doi: 10.1016/j.ypmed.2019.105770. Epub 2019 Jul 22. PMID: 31344384.
[AA] Wills TA et al. E-cigarette Use and Respiratory Disorder: An Integrative Review of Converging Evidence from Epidemiological and Laboratory Studies. European Respiratory Journal 2020; DOI: 10.1183/13993003.01815-2019.
[AB] Gotts JE et al. What are the respiratory effects of e-cigarettes? BMJ 2019; 366 :l5275 doi:10.1136/bmj.l5275
[AC] Tommasi S et al. A novel role for vaping in mitochondrial gene dysregulation and inflammation fundamental to disease development. Sci Rep 11, 22773 (2021). https://doi.org/10.1038/s41598-021-01965-1.
[AD] Davis LC et al. Predicting the pulmonary effects of long-term e-cigarette use: are the clouds clearing? European Respiratory Review Mar 2022, 31 (163) 210121; DOI: 10.1183/16000617.0121-2021.
[AE] Poonam Rao, Daniel D Han, Kelly Tan, Leila Mohammadi, Ronak Derakhshandeh, Mina Navabzadeh, Natasha Goyal, Matthew L Springer. Comparable Impairment of Vascular Endothelial Function by a Wide Range of Electronic Nicotine Delivery Devices, Nicotine & Tobacco Research, 2022;, ntac019, https://doi.org/10.1093/ntr/ntac019.
[AF] European Union. SCHEER (Scientific Committee on Health, Environmental and Emerging Risks), Scientific Opinion on electronic cigarettes, 16 April 2021. https://ec.europa.eu/health/system/files/2021-04/scheer_o_017_0.pdf
[AG] US Department of Health and Human Services. Smoking Cessation A Report of the Surgeon General. 2020. https://www.hhs.gov/sites/default/files/2020-cessation-sgr-full-report.pdf
[AH] US Preventive Services Task Force. Interventions for Tobacco Smoking Cessation in Adults, Including Pregnant Persons. US Preventive Services Task Force Recommendation Statement.JAMA. 2021;325(3):265-279. January 19, 2021 doi:10.1001/jama.2020.25019. https://jamanetwork.com/journals/jama/fullarticle/2775287
[AI] Quigley J et al. Electronic cigarettes and smokingcessation: An evidence review. Health Research Board. 2020. https://www.hrb.ie/fileadmin/2._Plugin_related_files/Publications/2020_publication-related_files/2020_HIE/Evidence_Centre/Electronic_cigarettes_and_smoking_cessation_systematic_evidence_review.pdf
[AJ] O’Brien D et al. Electronic cigarette use and tobacco cigarette smoking initiation in adolescents: An evidence review. May 2020. https://www.hrb.ie/fileadmin/2._Plugin_related_files/Publications/2020_publication-related_files/2020_HIE/Evidence_Centre/Electronic_cigarette_use_and_tobacco_cigarette_smoking_initiation_in_adolescents.pdf
[AK] Spain. Ministerio de Sanidad. Direccion general de salud publica. Inform sobre los cigarrillos electronicos: situacion actual, evidencia disponible y regulacion. 2020. https://www.mscbs.gob.es/ciudadanos/proteccionSalud/tabaco/docs/InformeCigarrilloselectronicos.pdf.
[AL] Banks E et al. Summary report on use of e-cigarettes and relation to tobacco smoking uptake and cessation, relevant to theAustralian context. 2020. https://openresearch-repository.anu.edu.au/bitstream/1885/211618/3/E-cigarettes%20smoking%20behaviour%20summary%20report%20final%20200924.pdf
[AM] Netherlands. Nationaal Expertisecentrum Tabaksontmoediging (NET). Trimbos Institutt. Facktsheet Elektronische Sigaretten (E-Sigaretten). April 2020. https://www.trimbos.nl/docs/160d6402-233a-426e-9343-b10d1c5f5b39.pdf
[AN] France. Haut Conseil de la santé publique. Avis. relatif aux bénéfices-risques de la cigarette électronique. November 2021. https://www.hcsp.fr/Explore.cgi/Telecharger?NomFichier=hcspa20211126_bnridelacileacdelavdufv.pdf
[AO] Health Canada. Risks of Vaping. Date modified: 2020-06-11. https://www.canada.ca/en/health-canada/services/smoking-tobacco/vaping/risks.html





